In the fiscal climate of 2026, the illusion of “good enough” billing is officially dead. While many organizations focus on front-end cash flow, a silent, systemic drain is gutting their net margins.
According to the latest Kodiak Solutions revenue cycle benchmarking analysis released in March 2026, U.S. hospitals and health systems lost a staggering $48.4 billion in net revenue in 2025 to final payer denials and uncollected patient debt. This represents a massive 25% increase in revenue leakage compared to 2024 (BusinessWire).
When revenue leakage grows by a quarter in a single year, legacy RCM models are becoming an active disinvestment in your organization’s clinical future.
The Anatomy of the Leak
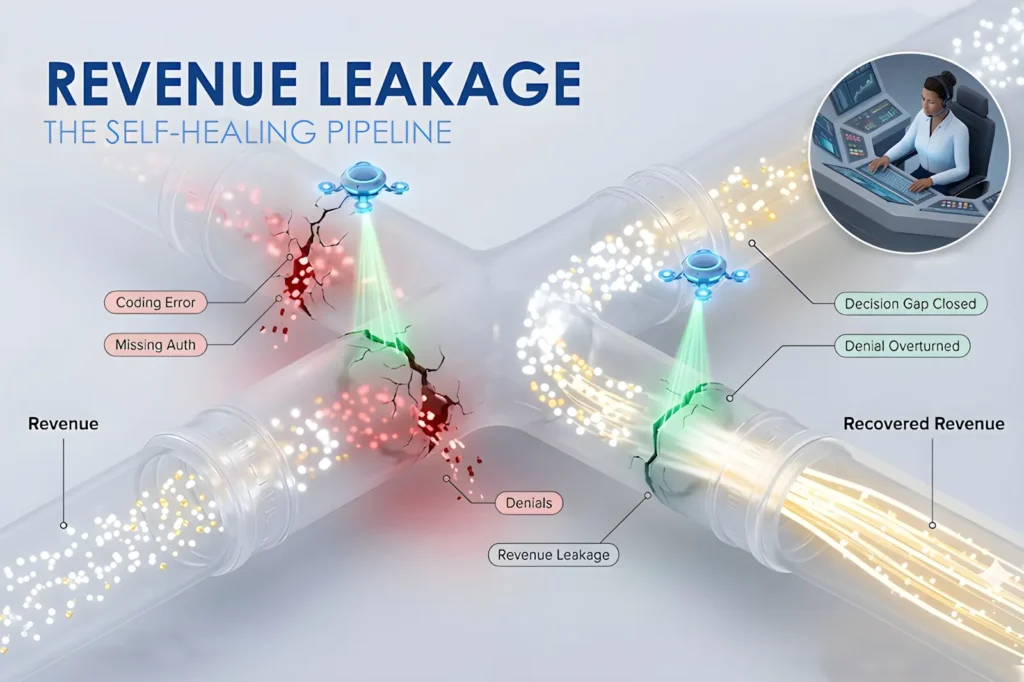
This isn’t your standard billing inefficiency. The current crisis is driven by three specific, high-friction “pressure points” that legacy teams are struggling to manage:
- The Rise of Clinical Denials: Payer behavior has shifted. Clinical Denials involving medical necessity and prior authorization accounted for virtually all of the increase in denial rates last year. Payers are deploying sophisticated automated denial engines, issuing “batch denials” within hours rather than days.
- The Patient Debt Trap: The patient responsibility share of net revenue rose to 7.3% in 2025, but collection rates on that share fell to just 42.4% (Fierce Healthcare). Without clear, culturally sensitive communication, this debt is becoming a permanent write-off.
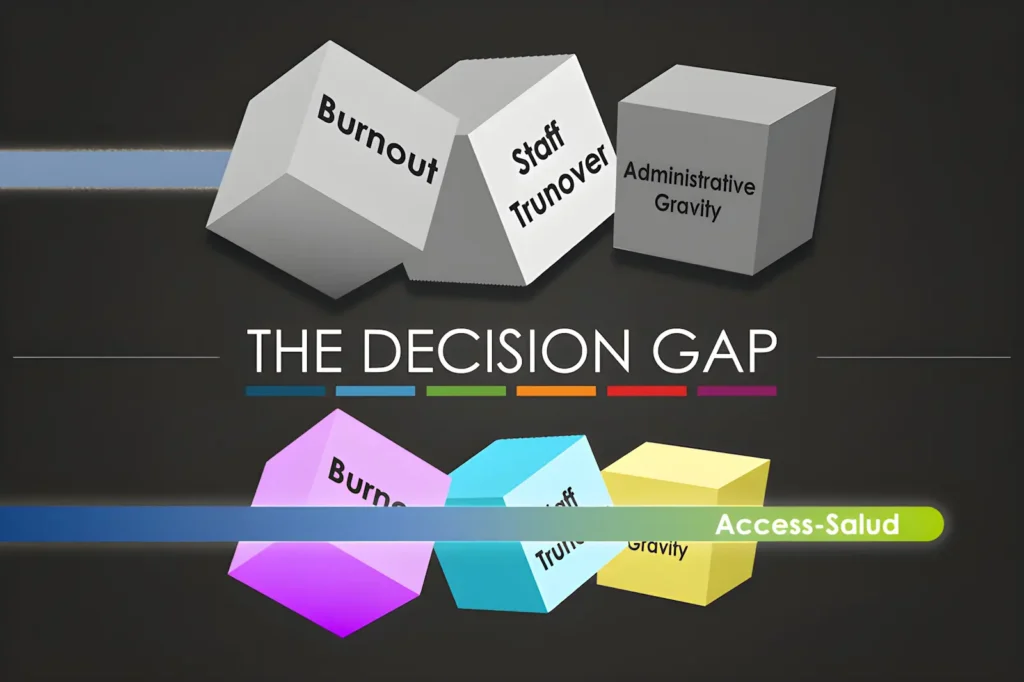
- Administrative Gravity & Burnout: A widening “Decision Gap” (the time it takes for a human to resolve a complex error) is exacerbated by a staffing crisis. Healthcare industry average annual workforce turnover reached 22.7% in 2025. The resulting “firefighting” environment creates a cycle of chronic stress that drains up RCM efficiency.
The Roadmap to Revenue Integrity
Stopping $48.4 billion tide a mental shift: from reactive billing to Revenue Integrity. Here is the gradual approach for 2026:
- Data Standardization: Compliance with USCDI v3 is no longer optional as of January 2026. Moving away from “free-text” coding to standardized data prevents technical denials before they reach the payer.
- Step 2: Cultural Synthesis (The Bridge): Revenue is recovered when patients understand their bills. Implementing bilingual, culturally sensitive support ensures that diverse patient populations understand their responsibilities, reducing uncollected debt by improving the patient financial experience.
- Step 3: Human-in-the-Loop Reasoning: Technology alone can’t win the “AI arms race” against payers. You need experts who can apply reasoning to complex clinical denials, identifying the nuances that automated systems miss (Centric Consulting).
The Turnkey Solution: Your Human Engine
Building a bilingual, USCDI-compliant, and burnout-proof RCM “War Room” is a massive, capital-intensive undertaking.
This is where Access-Salud steps in. We provide a synchronized nearshore team that acts as your Burnout Buffer. We don’t just process claims; we apply deep expertise and cultural understanding to close the “Decision Gap” in real-time.
By absorbing the high-friction administrative tasks, we allow your domestic leadership to maintain a Present Mind, focused on patients rather than paper.
[Schedule a strategic consultation with our Management Team today] to conduct a friction audit and reclaim your share of that $48.4 billion.





